Tags
I held off on writing about my follicle count during stims because I know how quickly it can change. But unlike last cycle, this one held pretty consistent. At each ultrasound I had 4 to 5 good size follicles and a few smaller ones. I kept hoping that the smaller ones would catch up. At my last ultrasound before egg retrieval, I had a solid 5 with 1 or 2 that might catch up in time, but I was told to not bank on those. I was actually okay with that going in and thought that perhaps my body was just putting in all the effort to grow these few high quality eggs, especially since we added in human growth hormone (HGH) for 6 days during stims to help with egg quality. Plus I’ve been on my egg quality cocktail of supplements – oh how I wish it was an actual cocktail – for so much longer at the time of retrieval. So I was ready for retrieval.
The anesthesiologist, however, was not. I sat there in the retrieval room, draped in paper gowns, and waited for this person to show up to my very important, and time sensitive, event. And then I waited some more. The RE assured me that I wouldn’t ovulate before retrieval because they calculate an extra couple of hours into scheduling specifically for uncontrollable events like this. Apparently there was a mix up with the anesthesiologists, or mine overslept – I’m not exactly sure. In an effort to get everything ready and save time while waiting on this person, a nurse came in to start my IV. She joked and said, “It’s okay, I’ve watch YouTube videos.” But then reassured me that she used to be a paramedic and I’m in good hands. Well I think dinosaurs must have roamed the earth back when she was a paramedic because the first attempt she hit a wall and the second and third attempts were blow outs. My husband intervened and told her not to try again and that we’d like to wait for the anesthesiologist.
I got a little break, then my RE came in and told me that he had a “plan B” – if the anesthesiologist is much later, they will give me “lots of pain meds and a little something to forget”. Now, I know he meant well, and honestly I’d do anything to get the eggs, but I couldn’t help but have a few tears start to fall. I was scared. I know some women do egg retrievals awake, but I’ve never heard a good story about it. It would hurt and I’m getting a little tired of all the pain involved in this process. This was not going how I expected! The RE also said that either way, we need to get the IV started. In came a different nurse who was able to get the IV going on the first try, though not without some struggle. And let me just mention that I have great veins. I’ve never experienced anything like this. To my relief, the anesthesiologist finally arrived in the nick of time and we didn’t need to revert to the dreaded plan B.
I was shocked to find that they retrieved 10 eggs! Some of my follicles contained 2 eggs (bonus!) and I guess some of the smaller follicles caught up. It was great news. My RE said he was hoping to get 5 or 6 embryos growing from these. Ahh, if only. As last cycle, my excitement only lasted a day until I got the fertilization report. The good news was that 9 of my eggs were mature, but the bad news was that only 3 fertilized with ICSI. And I was crushed. Again. I just don’t get it. How can my fertilization rate be so poor? I’ve been taking so many supplements, as recommended by my RE and consistent with the book, “It Starts with the Egg,” and we used HGH. What went wrong? This fertilization rate seems lower than would be expected for my age, and a drastic reduction from the 100% fertilization rate (natural – not ICSI) that I had at age 36. I know I’m 40 now, but that really does seem a bit much. I want to know why, but I’m trying to not focus on that right now, and hopefully I won’t ever have to.
Now I have 3 embryos growing. One of them has to be my golden egg. It only takes one. I focus on that, but it is so easy to get pulled back into the numbers game of probabilities and percentages. That’s a scary game. So I’m putting all my energy, prayers, and intention out to these little 3. Coincidentally, or not, I happened to have 3 egg shaped bees wax candles left from the bunch I bought when I started this journey. Bedazzled with green glitter, rose essential oil, symbols for protection and blessing, and sprinkled with the herbal mix I created when I set my intentions for this cycle, which you can find here, I mindfully light these three candles nightly to send this love and energy to my embryos. Tomorrow I will find out how they fared.


 By the time this lunar month comes to a close with the dark moon, I will have injected a full protocol of stimulation medications into my body, underwent another egg retrieval, learned how many eggs were retrieved, waited for and received the news of how many fertilized, found out how many embryos made it to biopsy for PGS testing and what quality they were, undergone two uterine biopsies for more ERA testing, and will be anxiously awaiting PGS results. Waiting on the fertilization report, embryo biopsy report, and PGS results will be some of the hardest parts to endure – far worse that what I will physically go though, which is by no means easy either.
By the time this lunar month comes to a close with the dark moon, I will have injected a full protocol of stimulation medications into my body, underwent another egg retrieval, learned how many eggs were retrieved, waited for and received the news of how many fertilized, found out how many embryos made it to biopsy for PGS testing and what quality they were, undergone two uterine biopsies for more ERA testing, and will be anxiously awaiting PGS results. Waiting on the fertilization report, embryo biopsy report, and PGS results will be some of the hardest parts to endure – far worse that what I will physically go though, which is by no means easy either. Supplies
Supplies I recently got back from a week long vacation. That never happens for us. Typically our only “vacations” consist of driving back to my hometown to visit my family. But we had an opportunity to join a couple family members at a cabin on Crescent Lake, Oregon. And for me, it was just what I needed after our failed FET. Time to get away from the stress of this process, spend quality time with my husband and daughter, and just simply relax in nature. Being in nature nourishes my soul. But there was one part of the trip that stood out among the rest in a very personal way – and surprisingly, it was when I was all alone.
I recently got back from a week long vacation. That never happens for us. Typically our only “vacations” consist of driving back to my hometown to visit my family. But we had an opportunity to join a couple family members at a cabin on Crescent Lake, Oregon. And for me, it was just what I needed after our failed FET. Time to get away from the stress of this process, spend quality time with my husband and daughter, and just simply relax in nature. Being in nature nourishes my soul. But there was one part of the trip that stood out among the rest in a very personal way – and surprisingly, it was when I was all alone.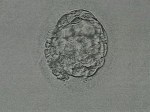


 I find that it’s so easy to over-analyze in this process, inevitable leading to anxiety. I’m also tempted to consult Dr. Google and we all know how that turns out. So I’ve been trying to not over think it, but the one aspect of my upcoming FET that has really got me in knots is the timing of the transfer and my Endometrial Receptivity Assay (ERA) results. Learning just enough about the ERA test and implantation to make me dangerous, I’m struck by just how small the window is for implantation. Since I only have one embryo, I know we have to get the timing right for success. When the timing is off, that’s when perfectly normal, healthy embryos don’t make it. Sure there are other reasons FETs can fail, but this is a big one. And so, I’ve been worried.
I find that it’s so easy to over-analyze in this process, inevitable leading to anxiety. I’m also tempted to consult Dr. Google and we all know how that turns out. So I’ve been trying to not over think it, but the one aspect of my upcoming FET that has really got me in knots is the timing of the transfer and my Endometrial Receptivity Assay (ERA) results. Learning just enough about the ERA test and implantation to make me dangerous, I’m struck by just how small the window is for implantation. Since I only have one embryo, I know we have to get the timing right for success. When the timing is off, that’s when perfectly normal, healthy embryos don’t make it. Sure there are other reasons FETs can fail, but this is a big one. And so, I’ve been worried. He drew a normal bell curve and explained that it represents how many receptors are active in the lining. The more receptors that are active (represented by the highest peak of the bell curve), the better chance an embryo has of implanting. The ERA results focus specifically on finding the peak window of receptivity – the optimal receptivity. This could be day 5 for some women, or other days like day 4, 6, or 7. My results gave a peak window on day 6, but there are still receptors active on day 5 (which for me would be on the right side of the bell curve where the line is lower), which is why my last IVF transfer worked. ERA doesn’t test for the whole bell curve – it’s aiming for the peak window. So he said, that this time I’ll have even more receptors active than last time so we will be giving my embryo an even better chance of implanting than we did the first time. That cleared up question #1 for me and made a lot of sense. Then he explained that the test is able to accurately calculate my receptive window even with the pre- and post-receptive findings, so they purposely space out the biopsies by 2 days (rather than doing days 5 and 6) to capture the best window. He said he is very confident in the results and that made me feel good too because he is great at what he does and I trust him. I’ve also read about the high accuracy of the ERA in research studies. That gave me peace of mind on question #2 also.
He drew a normal bell curve and explained that it represents how many receptors are active in the lining. The more receptors that are active (represented by the highest peak of the bell curve), the better chance an embryo has of implanting. The ERA results focus specifically on finding the peak window of receptivity – the optimal receptivity. This could be day 5 for some women, or other days like day 4, 6, or 7. My results gave a peak window on day 6, but there are still receptors active on day 5 (which for me would be on the right side of the bell curve where the line is lower), which is why my last IVF transfer worked. ERA doesn’t test for the whole bell curve – it’s aiming for the peak window. So he said, that this time I’ll have even more receptors active than last time so we will be giving my embryo an even better chance of implanting than we did the first time. That cleared up question #1 for me and made a lot of sense. Then he explained that the test is able to accurately calculate my receptive window even with the pre- and post-receptive findings, so they purposely space out the biopsies by 2 days (rather than doing days 5 and 6) to capture the best window. He said he is very confident in the results and that made me feel good too because he is great at what he does and I trust him. I’ve also read about the high accuracy of the ERA in research studies. That gave me peace of mind on question #2 also. Eight days until our frozen embryo transfer (FET). We’re almost there. I wrote in my
Eight days until our frozen embryo transfer (FET). We’re almost there. I wrote in my